The Diminishing Role of State in Healthcare
By Ayla Qayyum

Source: Samaa
Overview
The healthcare sector constitutes a major part of the policy arena in various countries. The state is involved in this sector in several significant ways; these include delivering healthcare services, regulating healthcare, taxing products with adverse health consequences, and providing health insurance.
Over the past years, there have been major developments in the public healthcare sector of Pakistan. In partnership with the World Health Organization (WHO), the State carried out initiatives to eliminate smallpox, guinea worm and malaria, and control tuberculosis and sexually transmitted diseases. The Expanded Program on Immunization was launched to decrease mortality caused by preventable diseases; thus, Pakistan’s under-five mortality rate declined from 181 in 1970 to 107.4 in 2006. Furthermore, Lady Health Worker Program was devised, which intended to deliver primary healthcare services to marginalized groups in rural and urban areas. The State also became a signatory body to achieve the eight United Nations MDGs to improve health indicators. However, several impediments plague the public sector.
Misallocation of funds
The State’s total spending on healthcare has been less than 1% of the gross domestic product over the past decade, whereas WHO recommends an allocation of 6%. Even with the outbreak of coronavirus disease, cumulative health expenditures barely reached 1.1% of the gross domestic product. To curtail problems in the public healthcare sector, State developed several programs to improve healthcare services. Although these led to an increase in patient satisfaction in some provinces, the funding of Rs. 20 billion was strikingly low, as compared to the scope of the activities.
Lack of good governance
In 2001, Local Government Ordinance was formed to place emphasis on accountability of citizens and participatory decision-making. Yet, due to the fragile capacity of the State, this objective remains unattained. Furthermore, corruption is widely entrenched due to a culture of patronage, unstandardized procedures for supervision, and safeguard of important decisions from scrutiny.
Inadequate delivery of services
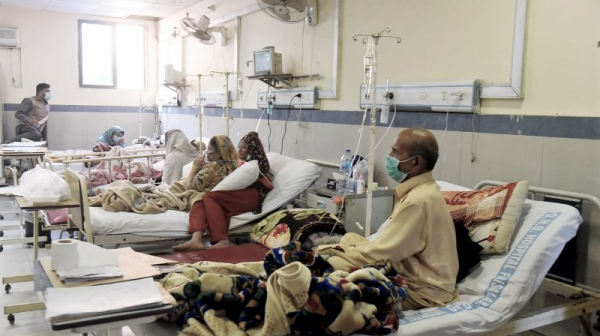
Currently, there is an epidemiological transition due to the soaring double burden of disease, including communicable and noncommunicable diseases. With 523,011 cases as of 19th January 2021, coronavirus disease has also put an unprecedented strain on the healthcare facilities. Furthermore, the rapidly growing population has resulted in a decline in the quality of service delivered.
Deficiency in human resources
As stated in the Punjab Economic Report of 2017, Punjab does not have an adequate number of medical practitioners to treat its population of 111 million; the doctor-population ratio is 1:1700, whereas WHO recommends a ratio of 1:1000. Overstaffing in urban regions, unfavorable recruitment policies and lack of performance-based incentives have also hindered efforts to instill motivation in the workforce.
Absence of research culture
Unavailability of accurate data and insufficient resources for research have led to a neglect of critical health issues that await well-articulated solutions. Even when research is conducted, it is futile as it does not have relevance to current matters. As a result, a weak informational base is formed, which creates a void between researchers and policy makers.
Proposed Interventions
The State should work on increasing the budget allocated to the health sector, as pledged in the country’s Vision 2025. A higher share should be ensured for essential services, preventive measures, and capacity-building of frontline workers. Moreover, ‘pro-poor’ programs, such as the National Health Insurance Scheme, should be given continuous funding.
Good governance is a critical step in bringing rapid improvements within the healthcare sector. There is a need to review the organizational structure and establish explicit accountability mechanisms. Moreover, key performance indicators and output based measures should be devised.
A high priority should be given to the research and collection of reliable data pertaining to operations within the sector. To monitor the overall performance, a Health Systems Database should be developed; this will allow users to analyse data and track the achievement of system-strengthening objectives. This will also allow the formation and implementation of technically sound policies.
Extensive retraining and capacity-building should be undertaken in order to achieve an optimal level of skills and motivation among the workers. Incentive packages, such as compensation for relocation and family reunion, should be introduced for service in ‘hard’ areas; this will attract qualified healthcare professionals and stem the trend of attrition. The State can also examine the possibility of utilizing the services of non-serving medical graduates, especially female doctors, who leave the profession due to personal exigencies.


